
In mid 2025, a male patient was urgently transported by Emergency Medical Services (EMS) to a partnering Emergency Department, where Sevaro serves as the hospital’s trusted neurology partner. The patient was found at home exhibiting classic signs of acute stroke: right-sided paralysis, facial droop, and expressive aphasia. Based on the estimated time of symptom onset, he was outside the therapeutic window for TNK (tenecteplase) administration.
Upon arrival, the stroke team conducted a rapid neurological evaluation, assigning the patient a National Institutes of Health Stroke Scale (NIHSS) score of 23; indicative of a severe stroke. The hospital’s Code Stroke protocol was immediately activated.
Within minutes, the patient underwent CT and CTA imaging. Results revealed a complete occlusion of the left M1 segment of the middle cerebral artery (MCA), confirming a large vessel occlusion (LVO)—a life-threatening condition requiring urgent intervention.
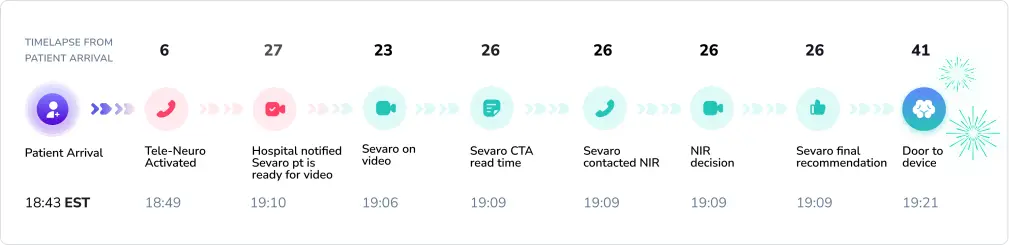
In this acute stroke case, Sevaro’s neurologist played a critical role in ensuring timely and coordinated care. Sevaro’s neurologist was on the video screen and prepared to assess the patient at the moment the patient arrived from the imaging suite, even prior to notification from the hospital staff eliminating any delay in evaluation or escalation of care.
CTA imaging was reviewed promptly upon availability, and Neurointerventional Radiology was contacted immediately based on the findings.
This real-time coordination and readiness supported rapid clinical decision-making and contributed to an excellent patient outcome. The case underscores the impact of Sevaro’s integrated technology and proactive clinical workflow in supporting hospital teams and optimizing stroke care delivery.
From door to diagnosis, every second counted — and our team delivered.
Once in the neurointerventional suite, the patient underwent mechanical thrombectomy.
Remarkably, the patient was discharged home just four days after arrival with a final NIHSS score of 0—indicating complete neurological recovery. This outcome underscores the effectiveness of a tightly integrated stroke response system.

This real-world case exemplifies the strength of a multidisciplinary, time-sensitive stroke care pathway. From EMS prenotification and Emergency Department triage to Sevaro’s remote neurology assessment and swift neurointerventional radiology (NIR) action, every phase of care was executed with precision. Seamless handoffs and synchronized teamwork ensured that no time was lost.
Key metrics:
NIHSS improvement: 23 ➡️ 0
This case is a testament to the power of collaboration, technology-enabled decision-making, and protocol-driven care. It highlights how a well-orchestrated stroke system can dramatically improve patient outcomes by turning a life-threatening event into a story of full recovery.
Q: What made this stroke case particularly high‑risk?
A: The patient presented with severe neurological deficits and an NIHSS score of 23, indicating a large, life‑threatening stroke caused by a complete occlusion of a major cerebral artery
Q: Why was thrombolytic therapy not used?
A: Based on the estimated time of symptom onset, the patient was outside the therapeutic window for TNK administration, making mechanical thrombectomy the appropriate intervention
Q: What role did Sevaro play in the patient’s care?
A: Sevaro’s consulting neurologist conducted rapid remote assessment, reviewed imaging in real time, and immediately coordinated with neurointerventional radiology to accelerate escalation of care
Q: How quickly was care escalated after imaging?
A: CTA imaging was reviewed as soon as it became available, and NIR was contacted within the same minute, eliminating delays between diagnosis and intervention.
Q: How did Sevaro’s technology impact response time?
A: Sevaro’s integrated platform enabled the neurologist to be live on video and ready to assess the patient before formal notification, supporting continuous momentum in care delivery
Q: What were the key performance metrics in this case?
A: Key metrics included a 33‑second initial response to Sevaro, immediate CTA‑to‑NIR communication, a 41‑minute door‑to‑reperfusion time, TICI 3 reperfusion, and full neurological recovery
Q: What was the patient outcome?
A: The patient achieved complete neurological recovery, was discharged home after four days, and had a final NIHSS score of 0, demonstrating the effectiveness of the coordinated stroke response
Q: What does this case illustrate for health systems?
A: This case highlights the value of a tightly integrated, technology‑enabled stroke care model where proactive neurology coverage and multidisciplinary coordination can dramatically improve outcomes